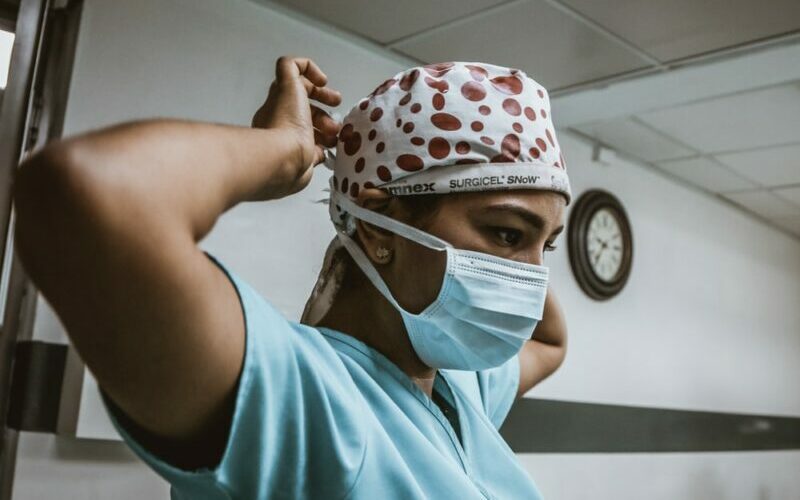
Front-line nurses, burnt-out or on the brink.
December 2, 2021
Pre-Covid, the healthcare system was already struggling. Its time to invest in primary care and best practices to take that weight off nurses.
Youre tired. Im tired. Everyone I know is tired. Everyone knows what has done it: almost 24 months of relentless Covid media, 11am announcements from the prime minister and premiers, rules, regulations, nasal swabs, isolations, vaccinations and lockdowns.
The whole world is tired and burnt out with it all, none more so than our front-line healthcare workforce and particularly nurses.
For two years they have been asked to hold the line, work in uncertain and often challenging conditions, masked, gowned and gloved-up, often alone with incredibly sick patients; they have being asked to show up in a system that even pre-Covid was struggling under the burden of chronic disease and poorly funded primary healthcare.
Two weeks ago, the ABC published “The burnout is ‘absolutely real’: A look at the state of Australia’s nursing workforce amid labour shortage”, canvassing two solutions to this pending burnout and potential mass exodus from the nursing profession: 1) more new graduates and 2) more overseas nurses.
Both solutions take time. The current burnout may result in an experienced nurses position being replaced by a new graduate or a recently arrived overseas nurse who, in terms of skill sets, would not adequately fill the void. I support both solutions in the longer term but there are more immediate, real-time actions that could lessen the impacts on our stressed and tired workforce.
Its time for leadership, not just management
Anyone in a leadership or management position must reflect on our everyday actions. Get out from behind our desks and speak and engage with our staff. Hear them (and let them feel heard), show empathy, be engaged and connect with them.
Give them some flexibility. If and when possible, review rosters (lets be fair and kind! Month on month of poor rosters wears everyone thin. If someone needs to take one for the team one month, be mindful for the next month.) We need to be hands-on and show we are willing to work with them, so they can find a place to revive and heal from two years of trauma.
Its time for leadership and not just management. Our staff need us more than ever and we need to be seen and they need to feel heard and valued. There are some exemplary practices out there but there is always room for improvement.
Enable full scope of practice
Throughout Covid we have left key healthcare practitioners on the bench, not utilising our valuable resources to the full scope of their intended and qualified practice (nurse practitioners for example). It’s time now to put politics aside and enable our nursing workforce to work to their full scope of practice and relieve the pressures felt across the system to empower and promote them, make them feel engaged and valued. For example, we are struggling to find workforce in regional and rural Australia in primary health care (PHC), yet we have nurse practitioners begging for opportunities to practise their advanced skills across the sector. Remove the red tape and let them work!
Bring the energy back
We need to remove the barriers to aspirational nurses who seek opportunity and development. Let us foster this, dont shut it down. Dont let years of service be the yardstick for promotion, training opportunities or leadership. Hire on potential, promote on attitude, foster and harness this energy.
When energy levels are down and people are tired, we can bring energy back to an overly bureaucratic workplace by finding, empowering, training, enhancing and promoting those bright stars. Now is the time to offer opportunity for development and to keep engaging and advancing our workforce.
I often come back to the question: Attitude is contagious is yours worth catching? Find that contagious, uplifting attitude, then foster and promote it. Others will follow.
Innovation and strategic partnerships
We dont need to do this alone, nor should it be done in isolation. Primary health care, community care, aged care and tertiary hospital care should innovate and collaborate, aiming for hospital avoidance and better chronic disease management in the community. These are critical mechanisms to reduce the burden on tired, overworked front-line workers.
Pre-Covid, the healthcare system struggled under the burden of chronic disease and emergency department waiting rooms full of people who could and should be served through available and willing primary care models. Its time to double down and invest in primary care and chronic disease management as a way of avoiding further burdens on tertiary healthcare workforce.
At the Rural and Remote Medical Service, for example, for more than two years we have been running a virtual GP service support for emergency department (ED) presentations in triage categories 35 (maximum waiting time of 30 minutes or longer) in the 33 hospitals in the Murrumbidgee area. We are a small charity that supports about 15 per cent of all ED presentations in the Murrumbidgee and we save the workforce time, workload and dollars in dealing with patients that dont need hospital-based care.
This service is scalable and with further scale we could reduce even more hospital presentations and the requirement for busy front-line workers to deal with patients that did not need the ED in the first instance. There are other similar hospital avoidance services; we need collaborative conversations to open doors and facilitate opportunities.
Medicare review
Better collaboration between primary care, community care and aged care can also go a long way to reducing barriers and burden on a single workforce. We need immediate funding modifications to enable such a collaboration and we also need to bring all parties to the table for blue sky thinking about what is possible in a healthcare world post-Covid.
There is no silver bullet for a burnt-out workforce and, it could be argued, those at the front line were feeling the pinch well before many of us heard of Wuhan, China. As we move out of fighting Covid into living with it, there is a real need for leadership, collaboration and integration. Bringing these together, we might just have the means to support our struggling workforce with reformed models of care that improve patient outcomes.