India's Coronavirus emergency tells a story poorly understood
May 5, 2021
The blanket and punitive travel ban for Australians returning from India is neither justified, nor does it make much sense in the efforts to curb the spreading of the virus. The Indian Coronavirus emergency is also raising many questions of the policies imposed around the world during the pandemic.
On 1 May, Health Minister Greg Hunt invoked, for the first time ever, emergency powers under the Biosecurity Act to stop travellers from India from entering Australia. Violators face five years’ jail and up to $66,600 in fines. This provoked outrage from human rights experts like former Race Discrimination Commissioner Tim Soutphommasane, media commentators normally associated with right-wing views like Chris Kenny, as well as Indo-Australians, for denying Australian citizens the inalienable right to return home and also for being racist in its selectivity.
When even Andrew Bolt says it’s difficult to explain the policy other than as racism, we have a problem. Figure 1 shows why the blanket ban on arrivals from India is not justified. Other countries in the chart, whose mortality rates were much higher at the peak of their Covid surge and people from those countries were coming to Australia in significantly greater numbers.
Of course, the reliability of all mortality statistics from India is suspect amidst such a massive calamity. But there is still no agreed definition and methodology for such key terms as tests, cases and what constitutes a Covid death. PCR and lateral flow tests are known to be very unreliable, with false positives and negatives common. This is why multiple negative tests are required to clear people suspected of having been infected and returning travellers in airport quarantine facilities.
Unlike the common flu, where only those who end up in hospitals are counted as ‘cases’, with Covid, anyone testing positive, including the large numbers of false positives, are commonly recorded as cases. It’s only after another year or more that we will be in a position to look at two-year trends and put all-cause deaths during the time of Covid into historical perspective, and then try to estimate how many died from and not just with Covid.
There are several additional features of interest about Figure 1. Within the global Covid envelope, India has often stood out as an anomaly, earlier with the puzzling low Covid casualties despite the extremely unfavourable initial conditions with respect to congested living and working conditions, more recently with the anti-seasonal surge of new double and possibly triple mutants.
Countries that experience an exponential growth in numbers killed with Covid always seem to experience a comparable rate of descent as well of their mortality curves, even in second waves. In contrast to all others in the chart, India did not experience an earlier exponential growth of infections, hospitalisations and deaths. This had bred hubristic complacency and the consequence has been tragic. Assuming Australia and New Zealand cannot close borders permanently to the rest of the world, have they done enough to build up hospital surge capacity to deal with nation-wide exponential growth of some new variant in the future or have they too succumbed to premature triumphalism?
Figure 1 also speaks to the reality that over a year since the declaration of the pandemic, no expert or government is on top of just how the virus behaves and how it is mutating, nor what is the best strategy to check and control it. At least to the point where we can all resume normal lives within an agreed state of endemic equilibrium where a certain level of risk from Covid is accepted.
For that reason, India’s current crisis must be placed both in international context and in relation to the totality of health threats to the lives of Indians.
With 1.83mn Covid deaths in the world in 2020, amounting to around 3% of all deaths in the calendar year, the disease is clearly deadly. Nevertheless, there were five killer diseases that were even deadlier: in ascending order, Alzheimer’s and dementia, influenza and pneumonia, lung diseases, strokes, and coronary heart disease, with the last causing 9.43mn deaths. This is why policy attention and public resources cannot be monopolised by Coronavirus but must scan the total public health horizon and establish a hierarchy of priorities that reflects the relative gravity of the different threats.
With 20 million total Covid-19 cases and 219,000 total deaths by 3 May, India’s numbers are the second and third highest in the world. On the daily new count, India is the worst hit on both key indicators. Yet, on cases and deaths per capita, India still ranks a lowly 114th and 116th (Table 1). Even against internal benchmarks, India’s average daily death toll is 25,000 from all causes. In the 12 months from 1 March 2020–30 April 2021, with 201,702 deaths Covid was the 13th biggest killer. Suicides numbered 287,435 and lockdowns are both a direct and indirect (’structural’) cause of suicides. The annual toll of traffic accidents, low birth weight, diabetes, diarrhoea, and tuberculosis ranged from 397,422 to 559,992.
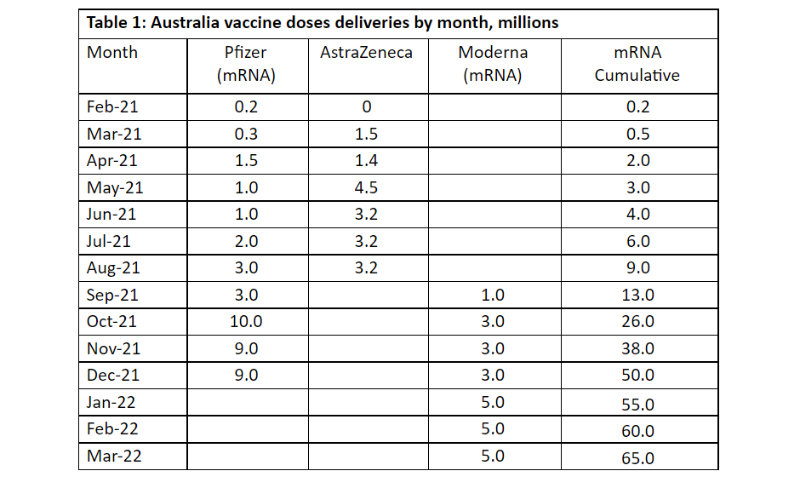
(Source Our World in Data)
Figure 1 is also graphic evidence of the policy-invariance of Covid-19 with regard to non-pharmaceutical interventions, where the infection, hospitalisation and mortality curves have followed their own logic and remarkably similar trajectories.
Over a year’s worth of actual data therefore have reconfirmed the scientific and policy consensus that existed before 2020, as faithfully summarised in the WHO report in October 2019 and also reaffirmed in the UK national pandemic preparedness plan as late as February 2020. Lockdowns can delay the spread of infections for a short time and this can be critical to ramping up hospital bed capacity and medical supplies, but they do not avoid the virus forever. The American Institute for Economic Research has compiled a list of 35 studies that show lockdowns are ineffective.
If lockdowns worked, Sweden would have a higher death rate than the worst-hit European countries and Florida would be far worse off than locked down California and New York. If anything, data indicate the opposite.
As can be seen in Figures 2 and 3, the curves of jurisdictions that locked down and those that did not follow a surprisingly similar trajectory. Figure 4 shows that US states that did not lock down for the winter are dispersed right across the mortality rates spectrum instead of being concentrated towards the higher end. On a per capita division, of the 2.2mn deaths for the US predicted by Neil Ferguson’s model of 16 March 2020 without mitigation, Florida with 6.46% of the US population should have had around 142,000 deaths owing to its lack of mitigation measures. Instead, on 30 April its Covid toll was 35,172.
Where the lockdown states and Florida do differ is in their social, economic and children’s education costs. Politico had a memorable headline on 23 December 2020: ‘Locked-down California runs out of reasons for surprising surge’. Experts were similarly puzzled by the failure of any post-holiday surge in Iowa despite dire predictions. In a MSNBC interview on 17 February, President Joe Biden’s coronavirus adviser Andy Slavitt visibly struggled to explain similar curves from lockdown California and no-lockdown Florida: ‘that’s just a little beyond our explanation’.
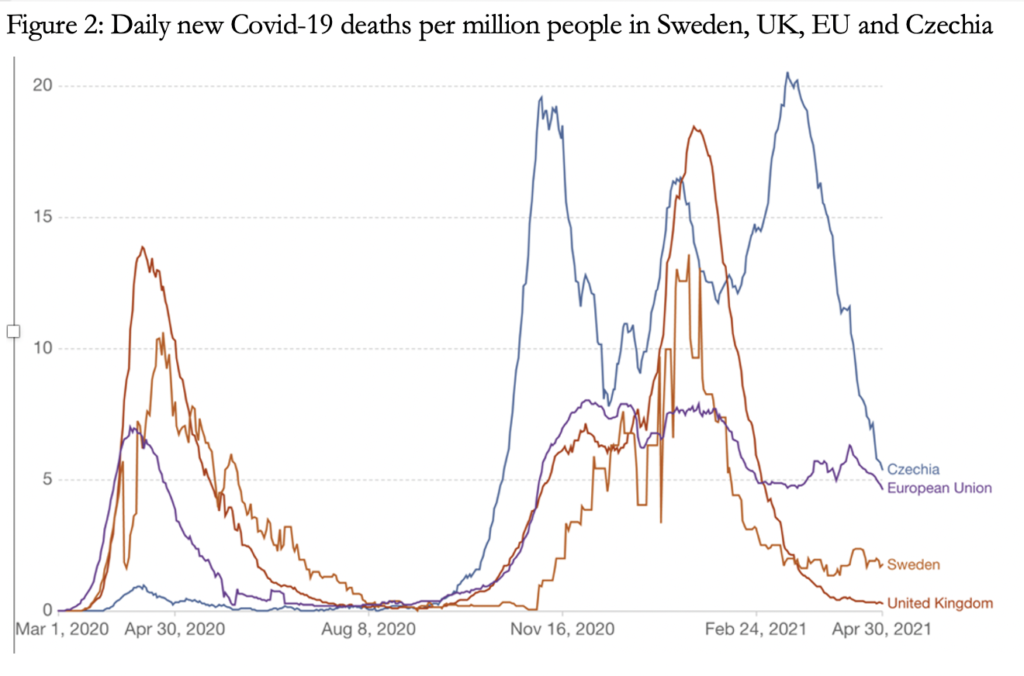
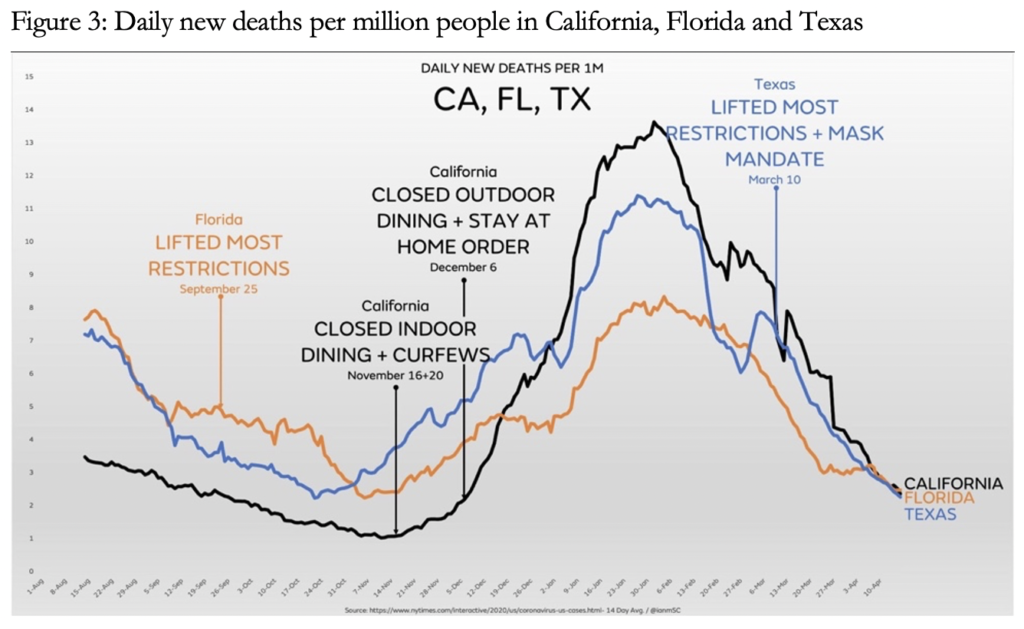
Against the questionable benefits of lockdowns, their immediate and lasting harm to health, mental health, livelihoods, social life etc. is immense, especially for the most disadvantaged and poverty-ridden groups and countries. A peer-reviewed article in the European Journal of Clinical Investigation by researchers from Stanford University in January 2021 showed that net harms exceed net gains between highly and less restrictive interventions.
Dr Sebastian Rushworth, a practising physician in a Stockholm hospital, reported in his well-regarded blog on a new study by Anna-Mia Ekström and Stefan Swartling Peterson of the Karolinska Institute. Using data from UNICEF and UNAIDS, they show that at least as many people have died as a result of lockdowns as of Covid.
The latter have died mostly in rich countries and been old, while most of those who have died of lockdown were younger people in poor countries who succumbed to malnutrition, lack of vaccination with childhood immunisation programs shut, and treatable diseases like TB and HIV. Considering their respective age-segregated mortality, the number of total years of life lost to lockdown is significantly greater than the number of years of life lost to Covid-19.
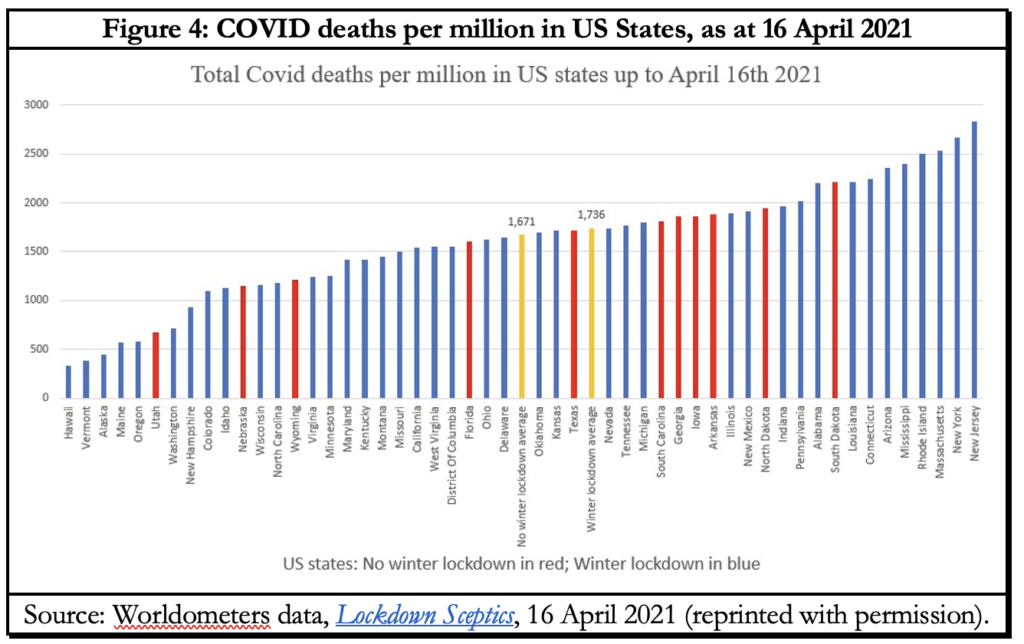
Four medical professors from Harvard, Oxford and Stanford Universities maintain a very informative website documenting the massive worldwide harm from lockdown measures, called Collateral Global, on physical, mental and social health, and on education and economy. Not coincidentally, two of the four professors, Jayanta Bhattacharya and Sunetra Gupta, are of Indian origin and therefore have a better idea of conditions in South Asia than most.
For example, lockdowns have forced 500mn children around the world out of school and more than half of them are in India. Pointing this out on the release of a new report, Dr Sunita Narain, Director General of the Centre for Science and Environment, said that similarly, more than half the world’s additional 115mn people pushed back into extreme poverty live in South Asia. India, she said, was all set to usher in a 375mn strong ‘ pandemic generation’ of children up to age 14 who are likely to suffer long-lasting impacts like increased child mortality, being underweight and stunted, and educational and work-productivity reversals.
Overall, then, the balance of risks and benefits varies between rich and poor countries and between those with good public health infrastructure and those without. Therefore authorities have to work out the best mix of mitigation measures for their own jurisdiction and not fall into the trap of ‘what’s good for Europe is good for India’ approach. One possible explanation for India’s sudden vulnerability to the double mutant could be the recommendation to wear masks in public.
After all, decades of ‘settled’ science before Covid-19 argued against their general use and it would be surprising to have that overturned so suddenly, especially with no gold-standard randomly controlled trials in the real world and not results from lab experiments using medical masks. Thus the UK’s pre-Covid national plan said that, public perceptions on facemasks notwithstanding, ‘there is in fact very little evidence of widespread benefit from their use’ in ‘the community and household setting’.
Figure 3 is a good representation of this abiding reality. Under Indian conditions, they may well have been seriously harmful. Photos and TV coverage on any day in different parts of the country show that substantial numbers of Indians are serial violators of critical mask protocols on hygiene practices, before putting them on and after taking them off, frequent fiddling with masks, lowering them below the chin, touching mouth, nose, eyes and face, single versus multiple use, discarding moist and wet masks, the incentivisation of risky behaviour like dangerously close physical proximity to others from the false sense of security given by masks, reducing distance between people because they cannot hear one another through masks, safe disposal, etc.
All this helps to explain why India has strongly resisted calls for another nationwide shutdown. In a sombre national address on 20 April shorn of his usual bombast and bravado, PM Narendra Modi said: ‘In today’s situation, we have to save the country from lockdowns’. He explained that current strategies to contain the rapid resurgence in infections were aimed at ensuring the least loss of lives and livelihoods, and appealed to states to consider micro-containment zones rather than lockdowns and encourage migrant workers to remain in situ with the assurance they would be vaccinated and not lose their jobs.
On 20 April, just under 10% of Mumbai’s 87,443 active cases were in slums and 90% in high rise and other mostly multi-storey buildings. Lockdowns are physically impossible in slums with multi-generational households sharing congested living conditions and communal washing and toilet facilities. The likely explanation for the tiny infection rate in slums is naturally acquired herd immunity. Conversely, lockdowns compel high-rise dwellers into more prolonged and acute exposure to pathogens than if healthy people were encouraged to spend time outdoors, especially in parks and on beaches, while maintaining physical distance and minimising human contact. Sick people should be told to stay home.
The crux of the problem in India is not the proportion of cases and deaths from Covid. Rather, it is the lack of a fit-for-purpose public health infrastructure and medical supplies of equipment and drugs. The Modi government has been no less negligent in this regard than its predecessors. But where previously the political, bureaucratic and financial elites have managed to circumvent the public system’s inadequacies by going private or abroad, Covid has caught them out with some viciousness.
More than anything else, the humanitarian tragedy blows apart the narrative of strongmen competence based on the pursuit of divisive and polarising policies to expand and consolidate political power.


